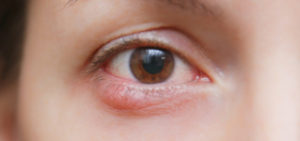
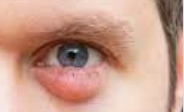
What is an eyelid lesion?
An eyelid lesion is a growth that develops on the eyelid, this can be a serious tumor or just a benign lump. Lesions may appear on the eyelid for a variety of reasons, including infection, benign and malignant tumors, and structural problems.
Most eyelid lesions are not vision-threatening or life-threatening, but should be evaluated by your eye doctor to ensure they are not cancerous, or pre-cancerous growths.
Proper treatment of eyelid lesions relies on an accurate diagnosis. Some lesions may respond to warm compresses and antibiotics, while others will require excision, cryotherapy or laser treatment.
There are two different types of eyelid lesions:
- Benign (noncancerous) eyelid lesions
- Malignant (cancerous) eyelid lesions
Signs and symptoms of an eyelid lesion
Benign (noncancerous) eyelid lesions may be pigmented or flesh colored, and often do not cause any pain or discomfort— unless they are scratched, in which case they may bleed and become painful.
Malignant (cancerous) growths on the eyelid can appear brown, black, red, or flesh-colored. These lesions may change in appearance, spread, or struggle to heal.
Malignant lesions may also appear with the following characteristics:
- Smooth, shiny, waxy
- Scaly, rough, red or brown patch
- Red and firm
- Bloody, crusty, or scabbed sore
- Flat, skin-colored or brown lesion
- Flat, scaly surface that is tender or itches
How are eyelid lesions diagnosed?
A comprehensive eye exam will provide the essential information required for an accurate diagnosis of an eyelid disorder.
The following factors should be investigated during the exam:
- The duration of the problem
- A change in size or appearance of a lesion
- Recurrence of a tumor that has been treated
- History of skin cancer
Your eye doctor will examine the structure of your eyelid, and look for signs of:
- Drooping
- Excess tissue
- Retraction problems
- Lesions
- Excessive tearing
- Misdirected eyelashes
Contact an eye doctor near you that will discuss the best options to treat any lesions on the eyelids.
SEE RELATED: What is a Stye?
Types of benign eyelid lesions
Seborrheic keratosis
Seborrheic keratosis is a condition that causes oily, pigmented lesions that appear to be stuck to the skin. They can occur anywhere on the skin, including the eyelids, and can become irritated. They’re most common in older adults, and can be removed surgically.
Actinic keratosis
Actinic keratosis is a lesion, or patch of skin that appears:
- Flat
- White
- Flaky
- Scaly
It occurs in sun-exposed areas and can be a precursor to carcinoma. A biopsy is usually performed to obtain more information about the lesion.
Nevus
Nevi are small lesions that appear at birth and are most commonly called moles, birthmarks, or beauty marks. They are well-demarcated, flat or elevated, and may be pigmented. They usually aren’t precancerous. However, junctional nevi, which occurs at the junction between the epidermis and dermis, can become malignant.
If you notice any changes in size or appearance, your eye doctor should evaluate it for melanoma and possible excision.
Xanthelasma
A xanthelasma is a soft, yellowish patch that appears under the lower fold of the eyelid. High cholesterol or genetic disorders can cause it to occur. Your eye doctor can remove it surgically, or by using a carbon dioxide laser.
Molluscum contagiosum
This condition occurs as a result of a viral infection and causes small, waxy nodules. It typically develops in people with weakened immune systems. If they occur near an eyelash, the nodules can cause inflammation of hair follicles. Your doctor can surgically remove or freeze the nodules, but they generally clear up without treatment as the viral infection clears up.
Hidrocystoma
A hidrocystoma is a transparent cyst located near the lid margin. It usually results from a blockage of the eyelid’s sweat glands. A surgical excision may be performed to clear the obstruction.
Types of malignant eyelid lesions
Basal cell carcinoma
Basal cell carcinoma is the most common type of cancer that develops on the eyelid. The tumor presents as a firm, pearly nodule, and usually appears on the lower eyelid or near the inner fold of the eye. If the tumor appears on the edge of the eyelid, eyelashes may fall out around the tumor.
Basal cell carcinomas can spread to other areas near the tumor, though they usually don’t metastasize. Large tumors may interfere with vision or eye movement.
Treatment of basal cell carcinomas generally involves surgery or radiation.
Small tumors can be removed with limited reconstruction. Large tumors require surgery and more complex reconstruction of the surrounding eye tissue. When surgery isn’t possible, radiation will be recommended— though it poses a higher risk of vision loss and higher recurrence rates.
Squamous cell carcinoma
Squamous cell carcinoma is less common than basal cell carcinoma, but it spreads more aggressively. Lesions generally form on the upper eyelid and frequently begin as actinic keratosis.
The lesion may appear:
- Raised
- Scaly
- Bloodshot
- Raw
Treatment is similar to basal cell carcinoma, though a more aggressive surgery is often necessary to eliminate cancer.
Sebaceous carcinoma
Sebaceous carcinoma looks similar to a chalazion or blepharitis and often occurs in older adults. This type of cancer aggressively metastasizes to other organs of the body. Because of its aggressive nature, large tumors of this type of cancer are best treated with total removal of the eye and its contents, to eliminate all of the cancerous tissue.
Melanoma
Melanoma is a rare pigmented eyelid tumor. These tumors are aggressive and often metastasize to the lungs and liver, even if they’re small. Melanoma is treated with aggressive surgery and radiation.
When to see an eye doctor
Schedule an exam with an eye doctor if you have noticed any growths or changes to the color or texture of the skin on your eyelids.
LEARN MORE: Guide to Eye Conditions
Through a comprehensive eye exam, your doctor will diagnose the type of lesion you are presenting with, and determine if further evaluation is necessary to rule out a cancerous or precancerous growth.
Treatment of eyelid lesions includes healing or removing the lesion— and greatly depends on the type of presenting lesion.