Have you heard your eye doctor mention ‘eye pressure’, but you are not really sure what it means?
Eye pressure, also called intraocular pressure (IOP) refers to the fluid pressure inside the eye. Maintaining a healthy IOP will help to preserve your vision and prevent vision loss from eye conditions such as glaucoma, a sight-threatening ocular disease.
How is IOP measured?
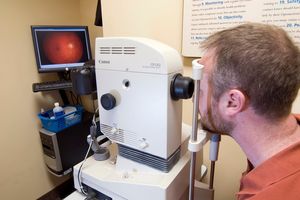
During a comprehensive eye exam, your eye doctor will perform a tonometry test to measure your IOP and detect any changes in your eye pressure. An increase in eye pressure can lead to optic nerve damage, and increase your risk of glaucoma.
Types of tonometry tests
Goldmann applanation tonometry test. This is the most commonly used test, as it is considered the most reliable way to measure IOP.
During this test, your eye doctor will place numbing drops into your eyes to ensure that the test does not cause any discomfort. Once your eyes are numb, a drop of non-toxic dye will be applied to your lower lid. You will then sit with your head positioned into a slit lamp device for proper lighting and magnification of your eye.
Your eye doctor will gently touch the surface of your eye, applying a minimal amount of pressure to flatten a small area of your cornea. Your eye pressure will be measured based on the amount of force needed to flatten your cornea.
Non-contact tonometry/ air-puff tonometry. This test is similar to the Goldmann applanation test, but uses a quick pulse of air to flatten a small section of your cornea.
Rebound tonometry. This test involves placing a small probe against your cornea and moving it slightly to measure your eye’s response to the touch. Certain devices that are used for this type of test, such as the iCare device, are portable and do not require numbing drops, and can therefore be used in the comfort of your home.
Tonometer or tonopen is another portable device that measures your IOP by touching your cornea and evaluating its indentation. However, this device requires numbing drops before the test is performed.
Does eye pressure remain constant throughout the day?
No.
It is important to understand that eye pressure varies throughout the day, and is usually highest in the morning. Therefore, measuring your eye pressure during an exam can only provide a small indication of your regular IOP.
Moreover, a fluctuation in IOP levels throughout the day can be dangerous to your ocular health, especially if you have glaucoma. Therefore, it is important to speak with your eye doctor to determine the best way to monitor your IOP— either at home, or during more frequent eye exams. Most of the time, eye doctors recommend measuring eye pressure in the morning, so keep that in mind when you schedule your next exam.
What causes an increase in eye pressure?
In a healthy eye, aqueous humor, or fluid, continuously moves through the eye.
Eye fluid is responsible for:
- Lubricating the muscles and fibers of the focusing lens
- Supplying nutrients and oxygen to the back of the cornea
- Clearing away waste products from the cornea
- Maintaining the shape of the cornea
As new fluid is produced, earlier fluid drains out through the eye’s anterior angle, where the cornea meets the iris. The fluid is sent from the eye to the uveoscleral drains and trabecular meshwork, down the back of the nose and throat.
This drainage system must remain clear and intact in order to maintain normal IOP. If a problem arises and the fluid is no longer able to drain efficiently, a buildup of fluid can occur, consequently causing an increase in eye pressure.
What happens when eye pressure remains high?
If your IOP remains high, between 15-25 mmHG, for an extended period of time without treatment, the pressure will continuously push on the optic nerve, causing damage— and consequently, permanent vision loss.
In some cases, a rise in IOP occurs suddenly, quickly exceeding 30 mm HG, or even reaching 40 mm HG. This is primarily caused by angle-closure glaucoma, or trauma to the eye, and can lead to severe optic nerve damage without any warning.
It is important to understand that changes in eye pressure do not cause any pain, and may therefore go unnoticed for years— while causing gradual vision loss.
Therefore, a tonometry test is crucial for detecting early signs of increased eye pressure, or ocular problems that may put you at risk of glaucoma. The sooner the disease is detected, the higher your chances for preventing vision loss, and/or preserving remaining vision.
Schedule an eye exam with an eye doctor near you who has experience in diagnosing and treating glaucoma.
SEE RELATED: Eye Emergencies
When should I have a tonometry test?
Tonometry testing is conducted during an annual eye exam, but may be conducted more frequently for the following reasons:
- If you are experiencing symptoms that may indicate a change in IOP
- If you are taking steroid medication post cataract surgery or for any other medical reason
- If you are at risk of glaucoma
- If you have been diagnosed with, or are at risk of developing iritis or retinal detachment
Which symptoms are associated with high IOP?
A variety of symptoms may indicate high IOP, but can also occur as a result of another ocular condition.
Therefore, if you are experiencing any of the following symptoms, your eye doctor will perform a tonometry test to rule out glaucoma:
- Severe pain
- Redness
- Blurred vision
- Halos around lights
- Gradual peripheral vision loss
- Tunnel vision
If you experience any of these symptoms contact an eye doctor near you.
Who is at risk of developing glaucoma?
If you are at an increased risk of glaucoma, a tonometry test will be conducted to detect any changes to your IOP.
Common risk factors include:
- Over 60 years of age
- African American or Hispanic race
- Family history of glaucoma
- Diabetes
- Hypothyroidism
- Chronic ocular conditions
- Eye injuries
- Myopia
- Extended use of steroid medication
What is considered a normal eye pressure?
Normal eye pressure ranges between 12 to 22 millimeters of mercury (commonly presented as mm Hg).
In most cases, if your IOP measures above 20 mm Hg, you may have, or be at risk of developing glaucoma.
However, in some cases, glaucoma can develop even with normal IOP— highlighting the importance of regular eye exams for the detection of any changes to your ocular health or vision.
In some cases, high IOP can occur following an eye injury, blood vessel inflammation, or other ocular problems— your eye doctor will look at other related factors for a proper diagnosis of an ocular condition.
LEARN MORE: Guide to Eye Exams
If you have a family history of glaucoma, or may be at risk of high IOP, contact an eye doctor near you to determine the most effective way to control your eye pressure, and reduce your risk of glaucoma.